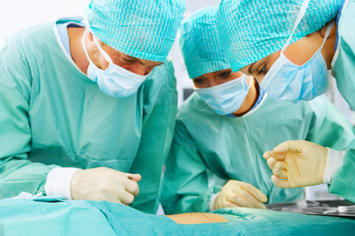
A Reuters article that was widely picked up around the globe recently raised the question, Are Doctors What Ails US Healthcare? Comparing the New York suburb of White Plains to Bakersfield, California, the article uses the evergreen two-Americas paradigm to discuss disparities in health care. Drawing heavily on the Dartmouth Atlas of Healthcare, it highlights a sad but inescapable fact: doctors want to live in some places and not in others, giving the “have” populations more intensive medical care which they might or might not need, while have-nots, who tend to be older, sicker and poorer, get health care to match. The article asserts that there’s nothing in current health care reform legislation that will do anything to address the disparities.
I agree. But then, what should we expect? The legislation, which I find marginally more desirable than doing nothing at all, is largely about insurance, not about health care. This is what happens when we emphasize how we pay for something, rather than what we are paying for. Are doctors what ails U.S. health care? Only in the sense that they are operating on the same basis as everyone else in the health care market: every man for himself.
You don’t have to make bi-coastal comparisons to find the disparities highlighted in the Reuters article. My own Hudson Valley not-for-profit insurance company faces them every day. We cover the Medicaid populations from the aforementioned White Plains, NY, to the South, to the blighted economies of the Catskills to the North and West. The distance involved is only about 150 miles, but day in, day out it might as well be 1500. And socially, it might as well be 150 years. Sullivan County is still organized geographically the way it developed in the eighteenth and nineteenth centuries — farms, woods, and mills, only without the mill jobs.
There was a brief shining moment (well, half a century) when urban Jews and other vacationers formed the basis of a thriving tourist trade in the “Borscht Belt” resorts of Monticello, Sullivan County’s hot spot. When they closed, they provided ideal settings for residential drug and alcohol rehab for poor people from New York City, but those aren’t exactly the foundation for high-quality community health care. When we initially started offering state-sponsored insurance to the poor of Sullivan County, the historical dearth of specialists made it a laboratory for what a free market looks like when there’s no competition. (Do I hear the words “strong public option”?) Because New York State requires us to have a decent network of contracted doctors for our enrollees, the sole cosmetic surgeon – for example – could extract pretty much any fee he wanted from us in exchange for seeing a patient who needed emergency reconstructive surgery.
Your tax dollars meet supply and demand and a mandate to pay within a private market.
I don’t blame the specialists. They are highly trained and skilled, and have paid their dues. If I blame anyone, it’s the system that sets the dues so high, in the form of college and medical school loans and years of fellowships that leave well-meaning doctors feeling that they deserve all that money, just like corporate farmers and hedge fund managers.
It’s also not the doctors’ fault that they want good schools and cultural amenities. I haven’t seen much of Bakersfield, but I know that schools in and around White Plains have good reputations and are just twenty miles from Broadway and the Metropolitan Museum (and ten miles from my Tarrytown office). Maybe we can fix schools and reinvigorate the National Endowment for the Arts to make every remote locale more like Westchester, but that would be socialism.
Dartmouth Atlas data is easily available online, and well worth spending some time with. You can use it to create all kinds of two-America scenarios that provide instant object lessons in our health care inequities. My personal favorite is that health care spending in Miami, Florida for Medicare patients in the last two years of life (highest in the nation) is exactly twice that in Portland, Oregon (lowest of the regions studied), with commensurate volumes of appointments, referrals, tests and hospitalizations, and no better outcomes. Here we see the same dynamics that make pawnshops spring up around gambling casinos and candy stores near public schools. Doctors go where the customers are, and once they arrive they maximize their revenues and measure success by volume, not outcomes.
Why should we expect anything different, when reform legislation is captive to the same kind of have/have not dichotomy that shapes health care delivery itself? Senators Max Baucus of Montana and Kent Conrad of North Dakota are two of the pillars of the anti-public option caucus. They come from states with small populations, and both take barrels of money from the health insurance industry because they can’t raise it locally. If they play their cards right, who knows? They could leave Congress and become haves themselves, like Billy Tauzin, who is now Big Pharma’s man in Washington, having engineered the passage of Medicare Part D, or Tom Daschle, once a champion of single payer, who now plays both sides of the street with special interest money.
Are Doctors What Ails US Healthcare? quotes David Goodman, Director of Health Policy Research at the Dartmouth Institute for Health Policy and Clinical Practice, who says there's an "irrational distribution" of the most valuable and expensive U.S. health care resources. I would say that the distribution is entirely rational given the insanity of the larger situation.
If we’re ever going to find our way out of this mess, we’re going to have to do for these health care backwaters, both rural and urban, what we used to do when private capital wouldn’t do the job. Set goals and build the infrastructure to serve them, because the market won’t do it. Want to electrify Appalachia? You need the TVA. Want to make the desert bloom? Build dams and aqueducts. Want to open up the interior of the country? Build an Interstate Highway system. Want doctors to practice in unattractive markets? Create an MD Bill for doctors like the old GI Bill for veterans, so that doctors emerge from training feeling more like public servants and less like indentured servants.
I attended a discussion of health care reform not long ago at the Yale School of Public Health. The representative of the private health insurance industry put the issues in a compelling perspective, although not, perhaps, for the reasons he cited.
His arguments were three: First, we require automobile owners to carry insurance, so requiring everyone to carry health insurance shouldn’t be a problem (I know that President Obama made this point, too, and I hated him for it). Second, do you want a health care system that runs like the Post Office, or one that runs like Federal Express? And third, the health insurance industry is really a jobs program, and do we really want to put all those people out of work?
These are shallow arguments. Car insurance? There’s no law that says you have to own a car, but everyone needs health care. A health insurance mandate is more like forcing every American to buy a new car and giving them a choice between Ford or GM. Post Office and FedEx? A company that can’t send a package overnight from suburban Tarrytown into New York City without round-trip flights to Memphis and back is no model for health care delivery, and besides, I’d like to see what FedEx can do for the price of first class postage. Jobs? A dynamic economy finds ways of redeploying redundant workers in more significant jobs. Wouldn’t those actuaries make good math teachers?
The arguments were so hollow that no one bothered to argue, and the insurance rep was undoubtedly relieved. A fellow panelist who practices medicine in Cambridge, Dr. David Himmelstein of Harvard, said simply, “My practice would have no trouble making money on Medicare, single-payer reimbursement rates if we didn’t have to pay so many people to argue with insurance companies.”
Unfortunately, the larger discussion is still stuck on insurance, and as long as it is, the two health care Americas will never become one.
Georganne Chapin is President and CEO of Hudson Health Plan, a not-for-profit Medicaid managed care organization, and the Hudson Center for Health Equity & Quality, an independent not-for-profit that promotes universal access and quality in health care through streamlining. Both organizations are based in Tarrytown, New York.












In a healthcare system we
In a healthcare system we are looking for better and advanced health opportunities through which we are able to repair our health care system; so government and health organizations are looking for promote and repair their health care system through effective health care reform program. The above article should be beneficial for us and provides a complete informative about health care reform.
urgent care Tucson
valuable post for me. As in
valuable post for me. As in I am planing for one of the treatments done to my body and after coming through this post, I think you have given lots of details is superb for me.
Cosmetic Surgeon
caucasian hair colouring
In healrhn care the key point is the location. Know all about it
caucasian hair colouring
Salon Singapore
Oxymoron?
Well,according to my opinion,Health Care Reform is "well meaning" but what I worry most about it is the quality of heath care going down... I can just see people being moved through clinics and the ER like a nothing. i don't want to be cynical about this but when it comes to individual insurance, "affordable plan" is an oxymoron. i have my first hair transplantation at http://www.AIHR.com.au last year and this insurance companies making me nuts.
True that health care is not
True that health care is not available to all equally but that is what the government has to ensure through its social health care policies and systems. Those who can afford expensive health care will always use it but those who cannot should be provided the same through a social health care system.
James